To learn more, HealthCare Business News spoke to Diku Mandavia, chief medical officer and senior vice president of FUJIFILM SonoSite, Inc and FUJIFILM Medical Systems U.S.A. in Bothell, Washington. Dr. Mandavia is also clinical associate professor of emergency medicine at the University of Southern California. He is a founding member and past chair of the American College of Emergency Physicians (ACEP) Ultrasound Section and the co-author of the ACEP Ultrasound Guidelines.
HCB News: How can ultrasound be utilized most effectively in the COVID-19 patient?
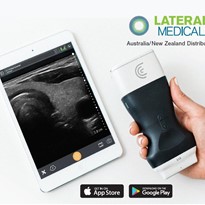
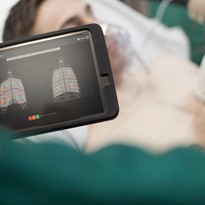
Dr. Diku Mandavia: COVID-19 is a respiratory virus that causes acute inflammation in the lungs, primarily seen as a patchy, interstitial infiltrate. Therefore, the point-of-care lung ultrasound exam is highly valuable and has already been shown in early clinical use to be very beneficial in recognizing these findings. For example, a small study by emergency physicians at Ospedale Guglielmo da Saliceto in Piacenza, Italy, published in Radiology, reported “strong correlation” between lung ultrasound and CT findings in patients with COVID-19 pneumonia, leading the investigators to “strongly recommend the use of bedside [ultrasound] for the early diagnosis of COVID-19 patients who present to the emergency department.” So, I would say that lung ultrasound is the top application, but these patients are also very sick: They may need venous access under ultrasound guidance to administer fluids and medications or they may be in shock and need a shock assessment, for which point of care ultrasound is also very useful.
HCB News: Why is point-of-care ultrasound better than computed tomography (CT) in the context of COVID-19?
DM: CT is a good test, but obviously is not a resource that is as readily available and often requires transport of a critically ill patient. Many of these patients are very hypoxic and ultrasound can identify the findings of COVID-19 at the point of care without having to transport an infectious patient out of isolation through hallways to a CT scanner, potentially leading to the need to disinfect the CT scanner, which the American College of Radiology has recently stated can take “approximately one hour.” All of these considerations mean that point-of-care has a convenience factor that is important in the context of COVID-19.














-160x160-state_article-rel-cat.png)