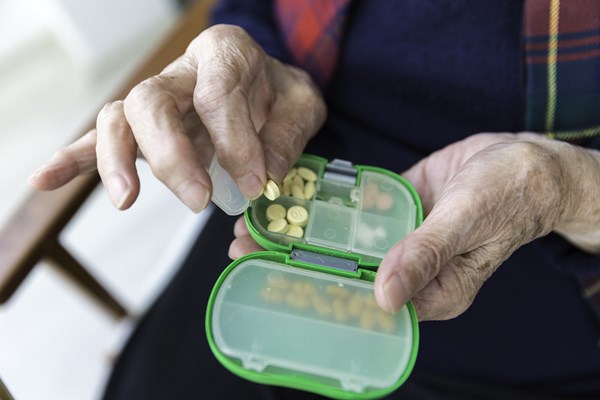
Older Australians may not be aware that they are on a ‘prescribing cascade’, where they take one medicine and have an adverse reaction, so are put on another medicine. One common example is when a patient is prescribed a nonsteroidal drug for pain, and is then prescribed a proton pump inhibitor (PPI) to reduce the risk of stomach side effects caused by the first prescribed medicine.
The new recommendations on appropriate use and prescribing of medicine include:
- recognising and stopping the prescribing cascade, to avoid adverse drug reactions in older people
- reducing the use of multiple medicines
- to not prescribe medicines without conducting a drug review, to avoid adverse outcomes for people on 5 to 20 medications, and
- to stop medicines when no further benefit will be achieved, particularly for older patients with a limited life expectancy where the treatments are unlikely to prevent disease.
Recommendations from the Australian and New Zealand Society for Geriatric Medicine include:
- do not use antipsychotics as the first choice to treat behavioural and psychological symptoms of dementia
- do not prescribe benzodiazepines or other sedative-hypnotics as first choice for insomnia, agitation or delirium
- do not prescribe antibiotics for asymptomatic bacteriuria in older adults
- do not prescribe medication without conducting a drug regimen review
- do not use physical restraints to manage older adults with delirium.
RACP President and The Australian and New Zealand Society for Geriatric Medicine (ANZSGM) member Dr Catherine Yelland says, "Care principles need to reflect the latest evidence and science, so that unnecessary tests, treatments and procedures are avoided. Equally important is the doctor-patient conversation to support informed and sound decision making to support high-quality care for older Australians.
"One of our recommendations is to not use antipsychotics as the first choice in treating behavioural and psychological symptoms of dementia, including aggression, resistance to care and disruptive behaviour. The use of antipsychotics is of dubious benefit and can lead to serious side effects that can be life-threatening. We recommend trying non-drug interventions first as they are an effective option. Ensuring a workforce is trained to be able to deliver nonpharmacological interventions is critical to being able to provide high quality care."
Professor Jennifer Martin from the Australasian Society of Clinical and Experimental Pharmacologists and Toxicologists (ASCEPT) (experts in the use and toxicity of medicines) says, "Many of our recommendations today will help patients avoid unnecessary tests and procedures and lead to discussions on reducing waste and overuse of medicines.
"One of our recommendations is to reduce the use of multiple medicines, common in older patients. Hyperpolypharmacy is where people may be on as many as 15 to 20 medicines at a time. Research has confirmed a significant association between polypharmacy and adverse outcomes among older people and an association with decreased physical and social functioning; increased risk of falls, delirium, hospital admissions and death. With an ageing population, use of many medicines at the same time is something we need to be having conversations about to avoid potentially harmful implications."
Dr Lynn Weekes, CEO of NPS MedicineWise who facilitate Choosing Wisely Australia says, "We are delighted to launch two more lists of Choosing Wisely Australia recommendations today. Choosing Wisely Australia is all about kick starting conversations about unnecessary tests, treatments and procedures, and that more is not always better. The adoption of these recommendations by health professionals will improve care.
"With the focus on medicines and older Australians in these lists, we urge people to consider if they are on the right medicine, or whether they could be taking too many medicines and if you are due for a review. It’s always timely to check with your doctor or pharmacist to see if any medicines are unnecessary and if they could cause harm if taken together."
To date, 98 recommendations have been released by Choosing Wisely Australia from 21 colleges, societies and associations, who have united for the initiative.
ASCEPT identified the following five recommendations:
- Recognise and stop the prescribing cascade
- Reduce the use of medicines when there is a safer or more effective non-pharmacological management strategy
- Avoid using a higher dose than is necessary for the patient to optimise the 'benefit-to-risk' ratio and achieve the patient's therapeutic goals
- Stop medicines when no further benefit will be achieved or the potential harms outweigh the potential benefits for the individual patient
- Reduce use of multiple concurrent therapeutics (hyper-polypharmacy).
ANZGM identified the following five recommendations:
- Do not use antipsychotics as the first choice to treat behavioural and psychological symptoms of dementia
- Do not prescribe benzodiazepines or other sedative-hypnotics to older adults as first choice for insomnia, agitation or delirium
- Do not use antimicrobials to treat bacteriuria in older adults where specific urinary tract symptoms are not present
- Do not prescribe medication without conducting a drug regimen review
- Do not use physical restraints to manage behavioural symptoms of hospitalised older adults with delirium except as a last resort. To read the lists in full, go to www.choosingwisely.org.au/recommendations