Osteoarthritis (OA) is a long-term chronic disease whereby deteriorating cartilage in joints leads to bones rubbing together, causing stiffness, pain, and reduced mobility. OA is the biggest cause of disability amongst older adults. It is estimated that 10-15% of all people aged over 60 have some degree of OA, with women more likely to suffer than men (1). Furthermore, the United Nations estimates that by 2050, 130 million people worldwide will be afflicted by OA, with 40 million severely disabled by the disease (2).
While the most severe cases of OA require surgical intervention, mild and moderate forms of the disease can be managed conservatively, with a range of electrophysical agents available to therapists to help patients reduce their pain and return to activity.
Breaking the viscious cycle of knee osteoarthritis
Along with the hands, feet, spine, and to a lesser extent the shoulders and hips, OA is most commonly found in the knees. The pain caused by knee OA can create a vicious cycle that is difficult for sufferers to escape. Once the pain becomes strong enough to stop the patient from moving, the resulting loss of circulation and muscle strength leads to reduced mobility, weight gain, and depression, all of which contribute to worsening of the condition and further pain, thus feeding back into the cycle.
Therefore, in order to break the cycle, the patient’s pain must be managed.
While not providing a cure, non-invasive conservative interventions for mild and moderate OA can reduce the progression of the disease as well as improving function and quality of life.
TENS for OA pain management
Although it cannot directly influence the degeneration of knee OA, transcutaneous electrical nerve stimulation (TENS) can provide pain relief to create a window of opportunity to allow for exercise, thereby delaying progression of the disease (3).
Unlike most other electrophysical agent interventions for OA, a portable TENS device can be used by patients in the comfort of their own home and has been shown to be a cost-effective way of improving quality of life for OA sufferers (4).
Muscle stim for OA
Neuromuscular electrical stimulation (NMES) mimics the way in which the brain sends signals to the muscles to make them work. Its ability to safely create stronger muscular contractions than would voluntarily be possible makes NMES a useful accompaniment to functional exercise for OA knee patients (5).
By stimulating the muscles with NMES during low-intensity exercises such as sit-to-stand, patients can strengthen their legs without putting undue stress on the knee joint. Furthermore, some multi-channel devices provide simultaneous NMES and TENS treatments, allowing the patient to relieve their pain as they exercise.
Ultrasound therapy for knee OA
There are currently 150 studies supporting the use of therapeutic ultrasound for improving pain and function in knee OA. While findings among these studies conclude that NMES is more effective for improving muscle architecture, ultrasound was found to be a better way of reducing pain and function (6). However, in order to enjoy the full benefits, patients will be required to undergo a significant number of ultrasound treatments.
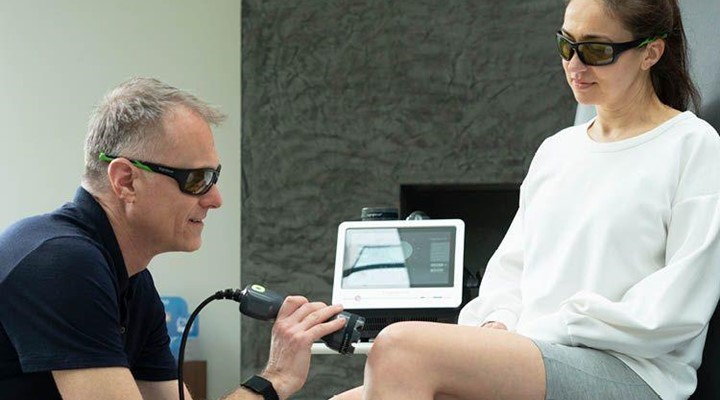
Laser therapy for knee OA
Photobiomodulation in the form of high power laser (HPL) therapy has been shown to be effective in reducing pain and improving function in patients with knee OA (7). HPL’s ability to provide an analgesic effect in short treatment times makes it both an effective and efficient option for managing the symptoms of knee OA and helping patients return to daily activities (8).
Furthermore, a study by Akaltun et al. (2021) showed that not only was HPL an effective modality on pain and functionality in knee OA patients, it also significantly increased the thickness of femoral cartilage.
Shockwave therapy for knee OA
Focused shockwave (F-SW) and radial pressure wave (RPW) therapies are also supported by a range of studies as an effective treatment for reducing pain and improving functionality in knee OA patients (10,11,12).
And while F-SW is considered by some to be preferable due to the improved comfort experienced during treatment, there is a growing appreciation amongst the scientific and physiotherapy communities for treatments involving a combination of both modalities. In such cases, F-SW can be used to treat the affected knee itself, while RPW can be used to treat the surrounding soft tissue.
To learn more about these modalities, reach out to your local representative.
References
- WHO Department of Chronic Diseases and Health Promotion. Available at: http://www.who.int/chp/topics/rheumatic/en
- United Nations. World Population to 2300. Available at: http://www.un.org/esa/population/publications/.../WorldPop2300final.pdf
- Chen, L. X., Zhou, Z. R., Li, Y. L., Ning, G. Z., Li, Y., Wang, X. B., & Feng, S. Q. (2016). Transcutaneous Electrical Nerve Stimulation in Patients With Knee Osteoarthritis: Evidence From Randomized-controlled Trials. The Clinical journal of pain, 32(2), 146–154.
- Woods, B., Manca, A., Weatherly, H., Saramago, P., Sideris, E., Giannopoulou, C., Rice, S., Corbett, M., Vickers, A., Bowes, M., MacPherson, H., & Sculpher, M. (2017). Cost-effectiveness of adjunct non-pharmacological interventions for osteoarthritis of the knee. PloS one, 12(3), e0172749.
- Benavent-Caballer, V., Rosado-Calatayud, P., Segura-Ortí, E., Amer-Cuenca, J. J., & Lisón, J. F. (2014). Effects of three different low-intensity exercise interventions on physical performance, muscle CSA and activities of daily living: a randomized controlled trial. Experimental gerontology, 58, 159–165.
- Devrimsel, G., Metin, Y., & Serdaroglu Beyazal, M. (2019). Short-term effects of neuromuscular electrical stimulation and ultrasound therapies on muscle architecture and functional capacity in knee osteoarthritis: a randomized study. Clinical rehabilitation, 33(3), 418–427.
- Wyszynska, J., & Bal-Bochenska, M. (2018). Efficacy of High-Intensity Laser Therapy in Treating Knee Osteoarthritis: A First Systematic Review. Photomedicine and laser surgery, 36(7), 343–353.
- Kim, G. J., Choi, J., Lee, S., Jeon, C., & Lee, K. (2016). The effects of high intensity laser therapy on pain and function in patients with knee osteoarthritis. Journal of physical therapy science, 28(11), 3197–3199.
- Akaltun, M. S., Altindag, O., Turan, N., Gursoy, S., & Gur, A. (2021). Efficacy of high intensity laser therapy in knee osteoarthritis: a double-blind controlled randomized study. Clinical rheumatology, 40(5), 1989–1995.
- Avendaño-Coy, J., Comino-Suárez, N., Grande-Muñoz, J., Avendaño-López, C., & Gómez-Soriano, J. (2020). Extracorporeal shockwave therapy improves pain and function in subjects with knee osteoarthritis: A systematic review and meta-analysis of randomized clinical trials. International journal of surgery (London, England), 82, 64–75.
- Zhong, Z., Liu, B., Liu, G., Chen, J., Li, Y., Chen, J., Liu, X., & Hu, Y. (2019). A Randomized Controlled Trial on the Effects of Low-Dose Extracorporeal Shockwave Therapy in Patients With Knee Osteoarthritis. Archives of physical medicine and rehabilitation, 100(9), 1695–1702.
- Xu, Y., Wu, K., Liu, Y., Geng, H., Zhang, H., Liu, S., Qu, H., & Xing, G. (2019). The effect of extracorporeal shock wave therapy on the treatment of moderate to severe knee osteoarthritis and cartilage lesion. Medicine, 98(20), e15523.